Polycystic Ovary Syndrome (PCOS) is a group of signs caused by a hormonal imbalance. It is very common, affecting between 5 and 10% of women and can be characterized by an unusual increase in the production of androgens (male hormones) in the ovaries. This syndrome impairs the growth of ovarian follicles and disrupts the production of eggs. It can increase the size of the ovaries [1].
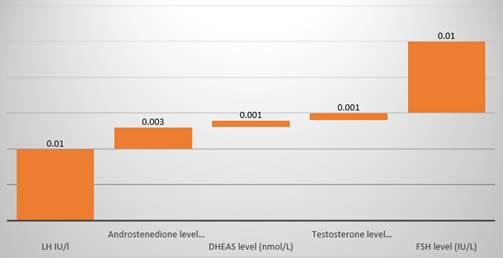
PCOS arises from a hormonal imbalance. Two hormones called FSH and LH (secreted by a gland at the base of the brain) regulate the ovarian cycle: their levels vary throughout the cycle, leading to ovulation.
In f PCOS, the level of LH often increases, which causes stimulation of the ovaries that produce excess androgens and impede the growth of follicles. The result: menopause. In addition, the level of testosterone rises in the blood, causing an increase in body hair and acne [2]. Finally, the level of insulin in the blood - a hormone used to regulate blood sugar levels - also tends to increase. However, if there is an overproduction of insulin, the body will secrete additional male hormones [3].
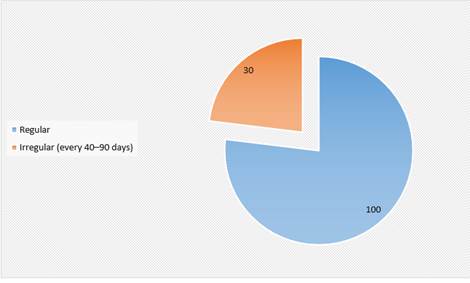
Polycystic Ovary Syndrome (PCOS) is one of the most common causes of infertility in women of reproductive age (up to 5-15% of cases). The main clinical manifestations of the disease are characterized by disorders of menstrual function of the type of oligomenorrhea, secondary amenorrhea, in some cases - menometrorrhagia as a result of endometrial hyperplasia, manifestations of androgenization of varying severity, overweight. Currently, there is a rethinking of the place of PCOS in the structure of endocrine pathology, considering it as a socially significant disease, given the direct connection between it with metabolic disorders (dyslipidemia, hyperinsulinism, insulin resistance, impaired glucose tolerance), leading to the development of arterial hypertension, abdominal-visceral obesity, early atherosclerosis, coronary artery disease hearts. Indeed, numerous epidemiological studies in various countries of the world have shown a high prevalence of PCOS among women of reproductive age up to 3-10% of the population [4]. The risk of developing myocardial infarction and ischemic heart disease in hyperandrogenism of non-neoplastic genesis is 7 times higher than in the general population of 40% of women.
There is increasing interest in the development of combined PCOS treatment regimens in which metformin a significant role is assigned [5]. Thus, it has been shown that the combined use of metformin (1500-1700 mg/day) and clomiphene citrate (100 mg/day) is highly effective by the method of induction of ovulation in PCOS This combination is prescribed in case of patient resistance to clomiphene, as well as the first stage of therapy in the presence of obesity, severe dyslipidemia, impaired glucose tolerance in PCOS. Another rational combination is the combination of metformin 1500-1700 mg/day and antiandrogen flutamide (125-500 mg /days), which leads to a synergistic effect about the normalization of the menstrual cycle, decrease in hirsutism, decrease in blood testosterone levels, decrease the amount of visceral fat, an increase in HDL levels Additional appointment to these drugs of low-dose oral contraceptives led to an additional increase in the level of CVH, which further reduced the index free androgens [6-10]. Thus, the use of metformin in the treatment of PCOS is a pathogenetic agent therapy aimed at correcting hyperinsulinism and insulin resistance, which leads to a significant effect about almost all clinical components of the disease (restoration of the menstrual cycle, induction of ovulation, reduction of hirsutism) and laboratory parameters [11,12].
Conventional treatment for PCOS includes:
Take contraceptives, which are usually recommended for women who are not planning to become pregnant. This approach is not a cure for PCOS, it masks symptoms and helps preserve fertility if a woman desires to have children in the future
Taking diabetes medications: Metformin, used to treat type 2 diabetes, maybe excellent for treating symptoms of PCOS. However, the use of this drug to treat PCOS has not been approved by the Ministry of Health
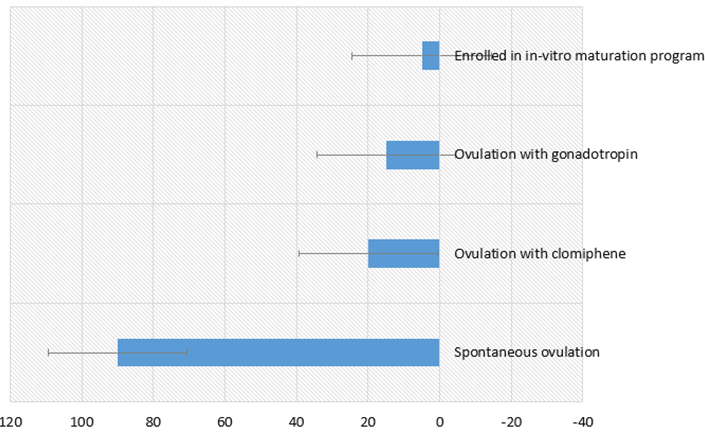
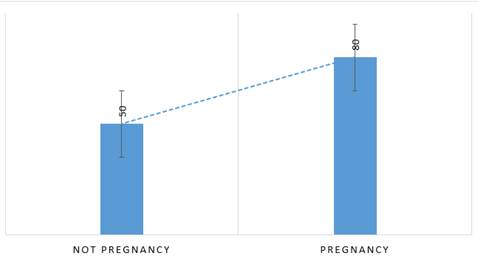
Preparations for infertility treatment (clomiphene (Clomid) injection, Gonadotropin) for women who want to become pregnant. Infertility problems in women with PCOS are associated with a lack of ovulationand taking these medications helps restore them